This playbook is for care delivery enterprise (health systems, hospitals, and ASCs) CIOs to leverage technology, particularly AI, to address four key existential challenges by their organizations: 1) revenue headwinds, 2) margin deterioration, 3) clinician shortages, and 4) patient expectations for speed, accuracy, and costs. It centers on AI as the core technology enabled by a new delivery paradigm framed by Services-as-Software™ (SaS).
Addressing these challenges with the specific steps in this playbook will yield tangible, quantifiable benefits such as increased revenue, reduced costs, improved clinician productivity, and higher patient engagement rates.
HFS Operational Playbooks are practical guides to solving key enterprise challenges that consume significant costs, time, and resources. The playbook provides enterprise leaders a realistic roadmap with specific “to-dos” to address their everyday challenges so they can clear mental and financial space to deliver next-level value.
The US healthcare delivery landscape, despite the enormity of AI-induced opportunities, is the most economically challenged industry segment. Externally driven headwinds include the One Big Beautiful Bill Act (OBBBA), which reduced Medicaid funding by close to 10% annually, slashed reimbursement rates across the board (primarily for Medicare), and a rapidly aging population with a high prevalence of chronic conditions that will continue to drive up the cost of care. Internally driven challenges include slow and low technology investments that prevent higher productivity and efficiency, unrealized benefits from M&A activities, and slow progress in finding new sources of revenue.
These challenges will manifest into four categories of threats that need immediate remediation. The rationale for urgency lies in the bleak data from the Cecil G. Sheps Center for Health Services Research at UNC, which identified 338 rural hospitals as particularly vulnerable. Other data points suggest that even urban and inner-city hospitals are vulnerable and at risk for closure.
Shrinking reimbursement rates by the Centers of Medicare and Medicaid (CMS), exacerbated by site-neutral payments, increased payer friction seen in higher rates of denied or delayed payments, prior authorization, and increased uninsured rates, are reducing the number of paying patients.
These factors will reduce revenues by 3% to 6% over a 12-month period and by 7% to 14% over a three-year period for those that survive this tsunami of challenges.
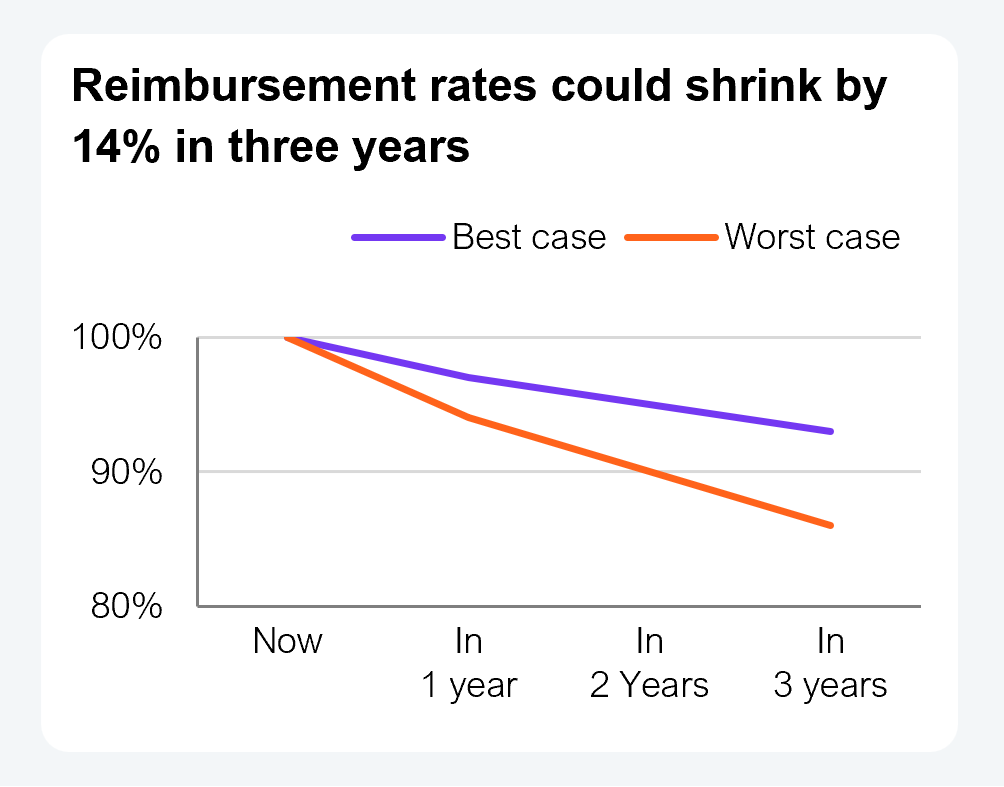
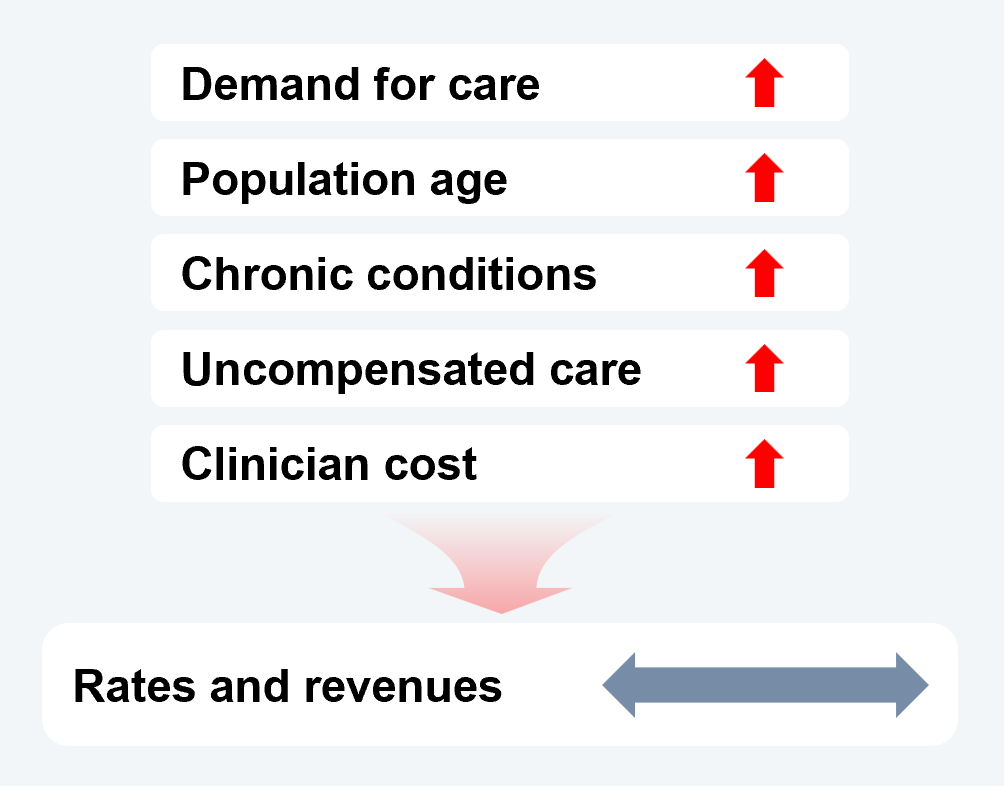
Demand for care will continue to rise as the population rapidly ages, bringing with it an increased prevalence of chronic conditions. Yet there will not be a commensurate increase in rates or revenues.
Increased uninsurance will triple the rate of uncompensated care, while the cost to attract and retain clinicians will grow only at rates above nominal inflation. Healthcare does not have a demand problem, just a monetization problem.
Burnout rates, slow speed to train replacements, and increasing demand for care are just some of the reasons clinician adequacy rates are likely to be in the high 80% range for physicians and in the low 90% range for registered nurses.
That rate will be worse for specialties most needed by the population based on demographics, such as primary care, geriatric care, and cardiology.

Despite rising uninsurance rates, consumers remain primarily in control of who they see for care and when. In that context, their evolving expectations for speed, accuracy, and cost are critical to understand and address. The Kaiser Family Foundation reported that 36% of adults in the past 12 months have skipped or postponed care they needed because of cost. Other data indicate that up to 50% of consumers will switch doctors if their expectations are not met.
These factors can cost as much as 4% of annual revenue over 12 months and will compound if left unaddressed.

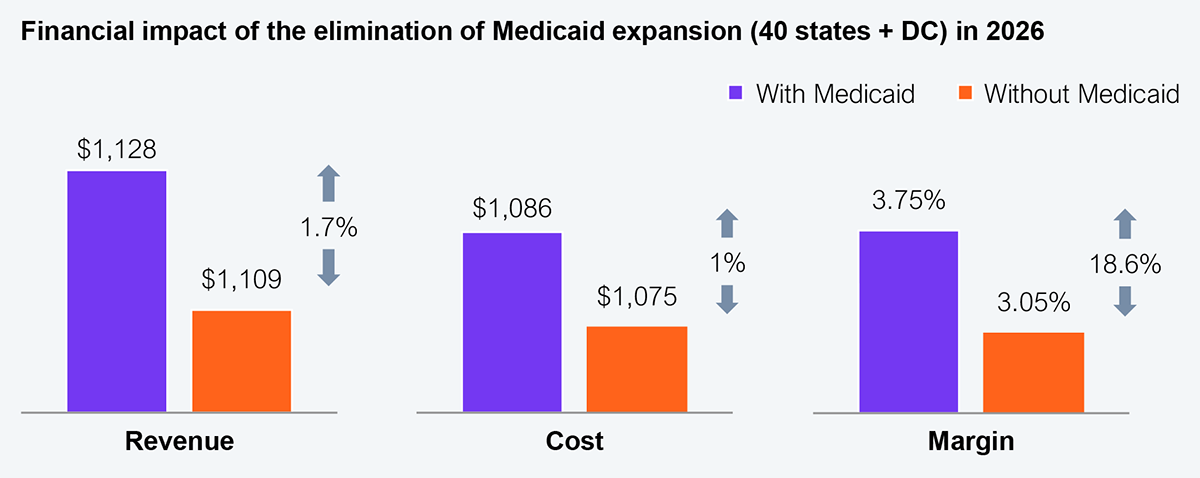
Source: Urban Institute, Commonwealth Fund, HFS Research, 2026
To read the complete report, click the download button below.
If you don't have an account, Register here |
Register now for immediate access of HFS' research, data and forward looking trends.
Get Started